Carrier spec updates, plan changes, feed monitoring, and technical troubleshooting are all included. Monthly fees cover ongoing support and system upgrades - no surprise charges, regardless of how many feeds you're running.
Carrier Connections - Live in 30 Days
carrier connections
you can count on.
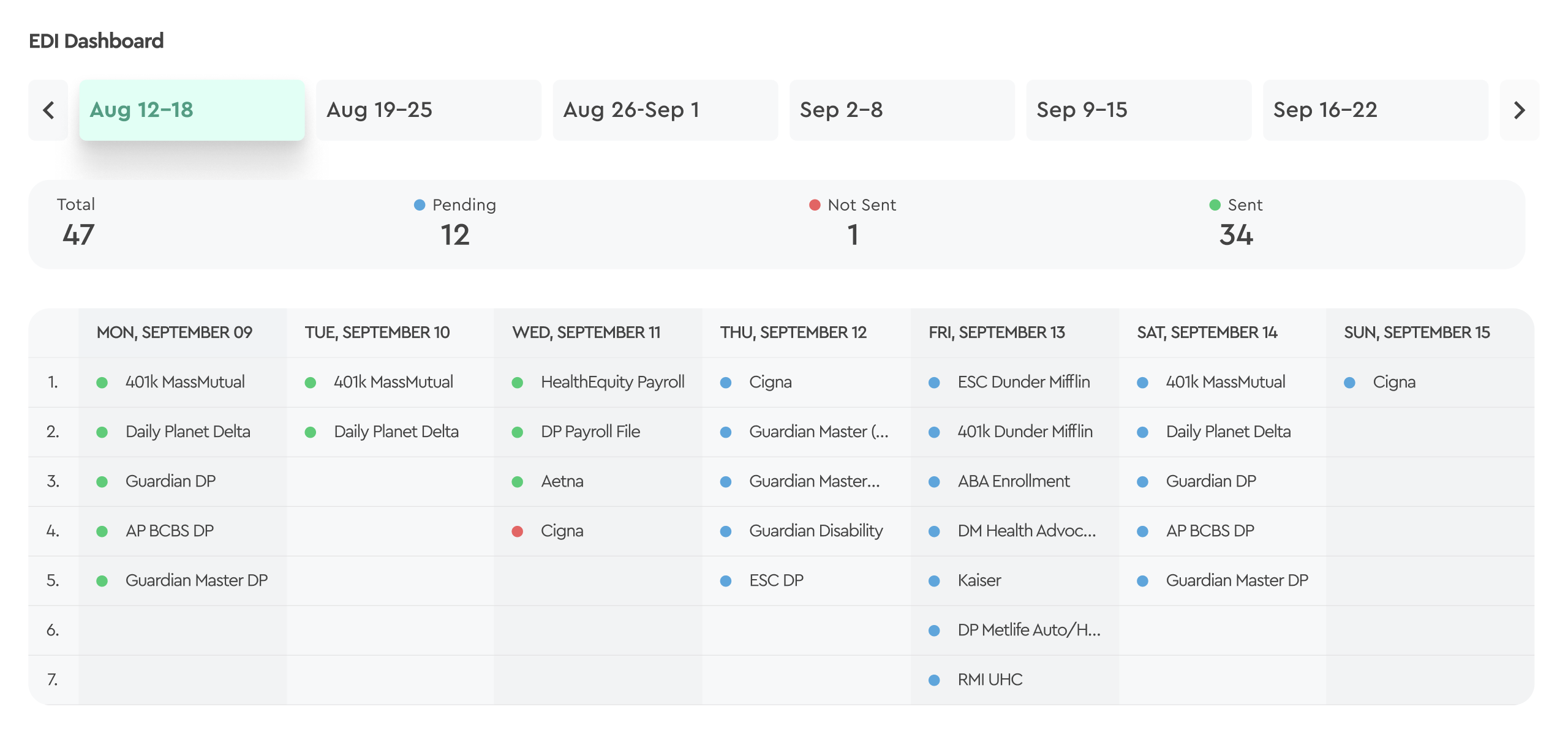
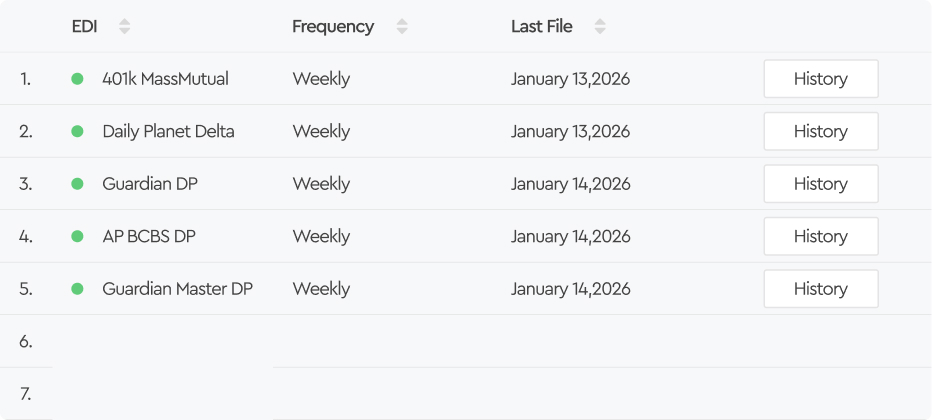
Tabulera handles your carrier connections end to end - white-glove EDI services plus software that gives you full visibility into every file.
Zero clients lost in 10 years
Providing Carrier Connections to world best teams