The biggest gap isn't speed - it's accountability. Spreadsheets have no audit trail. Tabulera logs every action across every stage, giving finance and compliance a defensible record of how every dollar moved.
Simplify Your Benefits Carrier Invoice Processing
Tabulera replaces the patchwork with one automated workflow. Enrollment data, carrier invoices, reconciliation, consolidated billing, and payments all live in the same platform - with one audit trail across the entire process.
How Benefits Carrier Invoice Processing Works in Tabulera
Each step in the workflow is handled by a dedicated module - automating the full process from enrollment to reconciliation.
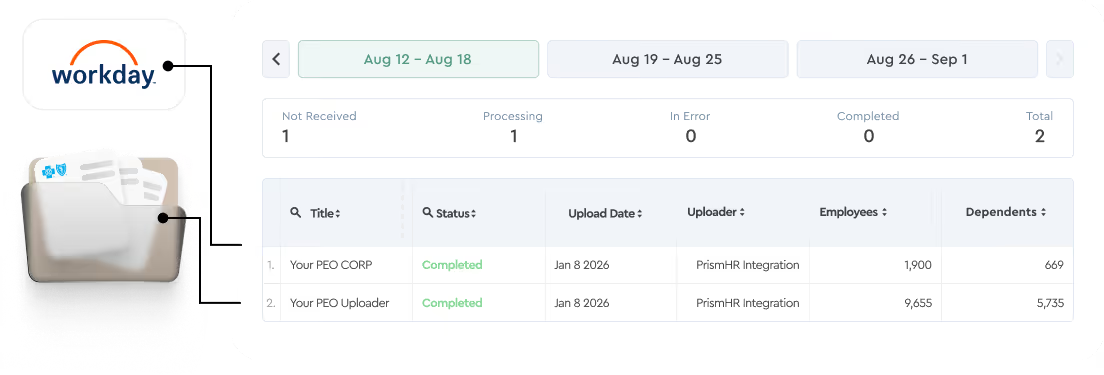
Data Intake
Enrollment, payroll, COBRA, and carrier invoices flow into Tabulera - feeding every downstream stage from a single dataset.

Enrollment Feeds
Tabulera transmits enrollment data to each carrier. Large groups use EDI Connectivity and small groups use Small-Group Data Transfers.
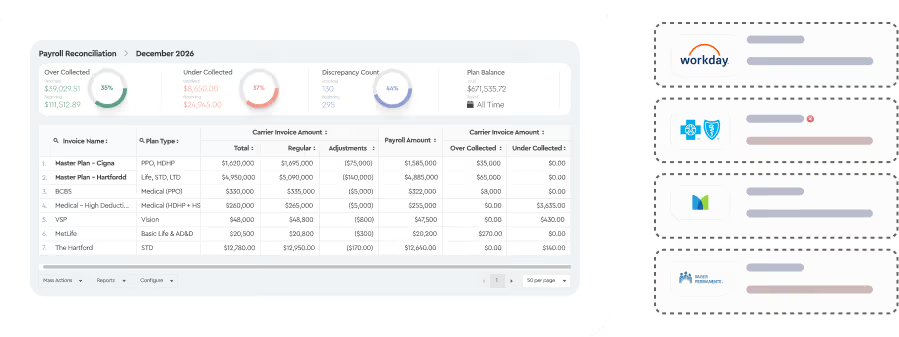
Invoice Reconciliation
Benefits Reconiliation module matches carrier bills against enrollment and payroll data - flagging wrong rates, terminated employees still being billed, missing coverage, and deduction mismatches.
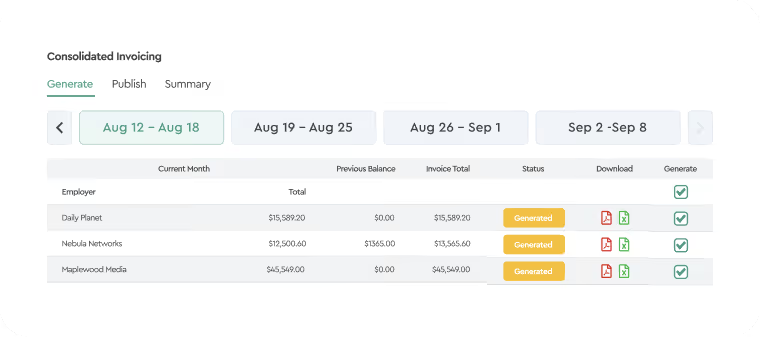
Consolidated Invoicing & Payments
The Consolidated Invoicing module combines multiple carrier bills into a single monthly bill, while the Payments module collects funds from each payer and distributes them to every carrier.
