Yes. Tabulera connects directly with PrismHR, isolved, Workday, Employee Navigator, ADP, UKG and any system that produces standard enrollment or payroll reports. No migration, no rip-and-replace. It fits the stack you already have.
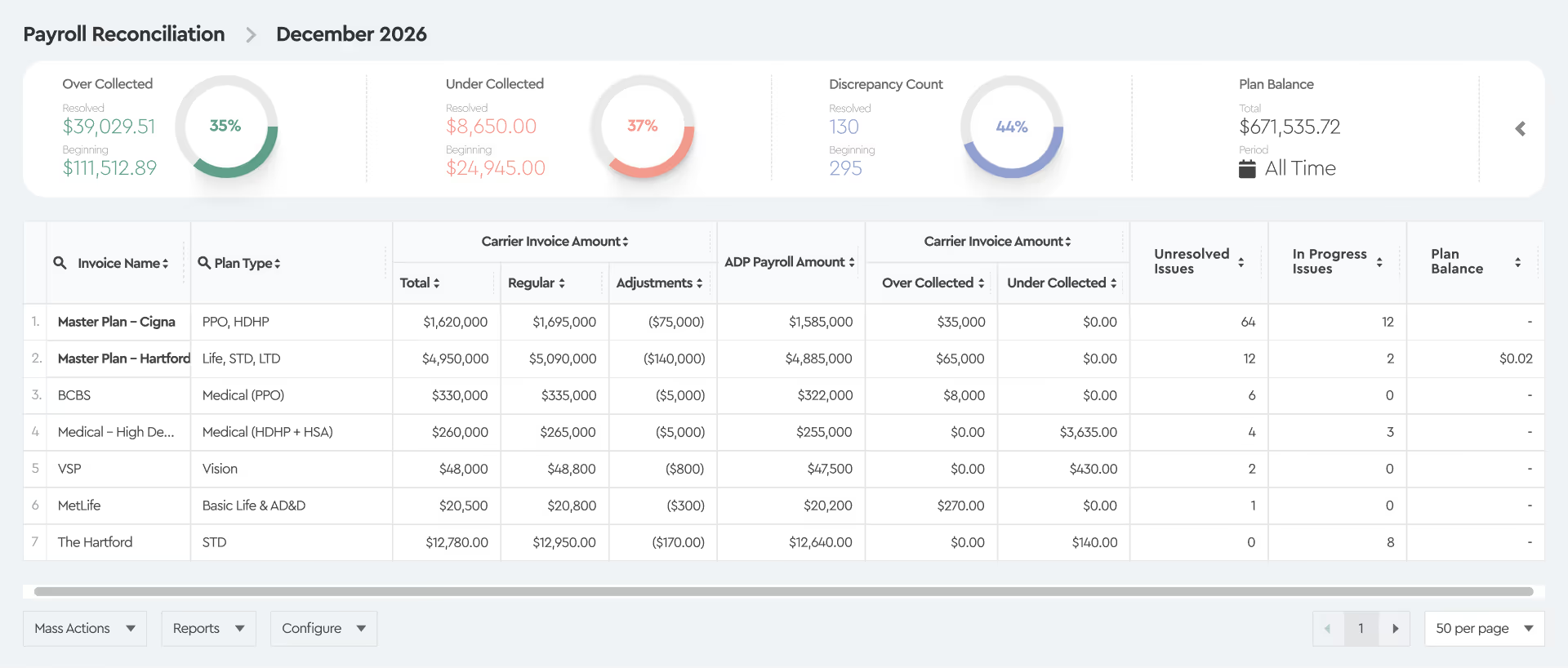
PEO Software for Benefits Reconciliation and EDI
behind leading PEOs
10+ years helping the leading PEOs stop premium leakage and deliver EDI files.
Trusted by: